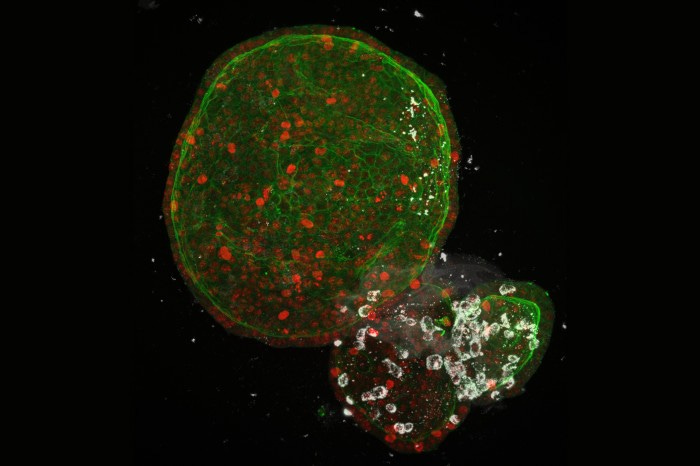
Human gut organoids infected with SARS-CoV-2 (white), the virus that causes COVID-19. Credit: Joep Beumer/Hubrecht Institute
One of the problems of medical research is that diseases and conditions like cancer vary from species to species, and experimenting with humans has severe ethical problems. A doctor isn't going to introduce cancer into a patient so he can study how cancers progress from stage to stage. Nor is she going to let a discovered cancer fester so she can watch it develop.
So researchers try to compare cancerous tissues from one person with healthy tissues from others. But researchers can't remove complete organs from a healthy individual, so they are restricted to small samples of tissue -- essentially studying healthy tissue in 2D. Scientists have long searched for a way to study healthy, human organs in 3D.
Stem cells gave us a tool.
Somatic cell nuclear transfer is a cloning method that can be used to create a cloned embryo for the use of its embryonic stem cells in stem cell therapy.[6] In 2006, a Japanese team led by Shinya Yamanaka discovered a method to convert mature body cells back into stem cells. These were termed induced pluripotent stem cells (iPSCs).
Originally stem cells got a bad reputation because they were developed from tissue from abortions. Finding a way to develop stem cells from adult tissue was critical for researchers. It is from adult, healthy and diseased tissues, these stem cells organoids are developed. What are organoids?
Organoids are tiny, self-organized three-dimensional tissue cultures that are derived from stem cells. Such cultures can be crafted to replicate much of the complexity of an organ, or to express selected aspects of it like producing only certain types of cells.
These solve the 2D problem of tissue samples. Small human cells are developed in the lab that replicate human tissue. These can be lungs, hearts, brains or other tissue.
An example of how this works:
Shuibing Chen spent close to two months tending to her mini lungs — some half a million of them. Each one looked like a tiny storm cloud, ensconced in a warm dish and protected by a jelly-like dome. Chen, a stem-cell biologist at Weill Cornell Medicine in New York City, and her team had nurtured them from clumps of human cells, adding nutrients every few days as they grew into 3D air sacs.
These lung organoids matured until they reached the size of a lentil. Then, the team packed them up and transported them just a few blocks away, to a laboratory authorized to work with SARS-CoV-2, the virus responsible for the COVID-19 pandemic. There, the organoids were drowned in virus and each was doused with one of 15,000 drugs. Almost all of the mini lungs died, but a few of the drugs stemmed the infection — representing a handful of possible treatments for COVID-19.
This gets around the ethical problem of experimenting with real humans. Researchers are using lab grown lungs to research how COVID-19 in its various flavors, Omicron and others, attack lungs. The lungs are the first major organ that COVID attacks after it enters through the mouth and nose. Stopping it there is critical.
There are some illnesses that are hard to study.
Before she started working with organoids, virologist Mary Estes relied on a much messier way to study the highly contagious vomiting bug norovirus. Nobody could grow the virus in the laboratory. So instead, she would isolate it from the excrement of people who willingly ingested it — and suffered the consequences — for the sake of her research.
In 2011, she saw a paper by Clevers [Hans Clevers, a developmental biologist at the Hubrecht Institute in Utrecht, the Netherlands] in which he grew mini guts from stem cells scraped off the villi, the tiny tentacles that line people’s intestines1. Clevers had created the first organoids derived from adult stem cells, which grow almost indefinitely under the right conditions, and can build themselves into complex structures that reflect their organ of origin. (Organoids had already been made from embryonic stem cells or induced pluripotent stem (iPS) cells, which can develop into any cell type, but they typically reflect organs early in fetal development.)
Organoids are proliferating in cancer research.
Despite significant strides in multimodal therapy, cancers still rank within the first three causes of death especially in industrial nations. A lack of individualized approaches and accurate preclinical models are amongst the major barriers that limit the development of novel therapeutic options and drugs. Recently, the 3D culture system of organoids was developed which stably retains the genetic and phenotypic characteristics of the original tissue, healthy as well as diseased.
The finding that organoids can also be established from tumor tissue or can be engineered to recapitulate tumor tissue has dramatically increased their use in cancer research.
They are even working their way into brain research -- a much tougher target as the brain is made up of many different types of tissue.
The culture of EBs [embryoid bodies] in the spin bioreactor spinning system encourages proliferation and differentiation into brain organoids representative of specific brain regions.
Organoid development will come out of universities and migrate to small companies. It will take some time. If you are going to keep an eye out for medical developments, organoids is certainly one of the areas to keep watching. Companies will begin specializing in different forms to be used in research. You will need to take several small positions in promising companies. It's the kind of development that will lead to single winners in a field like lung organoids.
Organoids will become an important part of medical research. Don't ignore them.
Please forward to interested third-parties. If you wish to have the regular Wednesday Musings in your email box, but aren’t ready for a paid subscription, just click on “Subscribe” and select “none”. If you are one of the few who wish to sponsor my effort, bless you. But you get the same messages as everyone.
I try to answer all questions or comments.